Don’t feel like having a big Q-tip shoved up your nose to be tested for COVID-19? Want to be tested from the comfort of your own home? Well, there is an at-home saliva test available from multiple sources, including Costco and Vault Health. The negative is that it will likely run you about $120 and it could take a few days to get results, but given the wait times for swab tests lately it might be worth considering.
Tag Archives: covid-19
1NT: Hunger and the Pandemic
11% of US households were food insecure before COVID-19 outbreak; by late April, within 1 month of the start of lockdowns, the rate had doubled to 22.7% – Source: November, 2020 issue of Rotary Magazine
Sobering
For the day job, I get to see lots of reports and data, particularly as it relates to housing. It was one of those reports that had a link to the US Census Household Pulse Survey pageand let me tell you that you’ll find some sobering statistics there about the impact of COVID-19. The survey has been conducted weekly since March 13, 2020, and below are select numbers from week 12, the most recent week available:
Employment Income – Percentage of households that had experienced a loss of employment income:
United States: 51.1%
North Carolina: 45.7%
Expected Loss in Employment Income – Percentage of adults who expect someone in their household to have a loss in employment income in the next 4 weeks:
United States: 35.2%
North Carolina: 29.0%
Food Scarcity- Percentage of adults in households where there was either sometimes or often not enough to eat in the last 7 days:
United States: 12.1%
North Carolina: 11.8%
Delayed Medical Care – Percentage of adults who delayed getting medical care because of the COVID-19 pandemic in the last 4 weeks.
United States: 40.1%
North Carolina: 33.9%
Housing Insecurity – Percentage of adults who missed last month’s rent or mortgage payment, or who have slight or no confidence that their household can pay next month’s rent or mortgage on time.
United States: 26.5%
North Carolina: 23.0%
K-12 Educational Changes – Percentage of adults in households with children in public or private school, where classes were taught in a distance learning format, or changed in some other way.
United States: 99.4%
North Carolina: 99.7%
About That Family Gathering
Catawba County (NC) recently published a case study to show how one family gathering of over two dozen people ended up with 14 family members infected with COVID-19 who then spread the infection to 41 people in 9 different families and 8 different workplaces.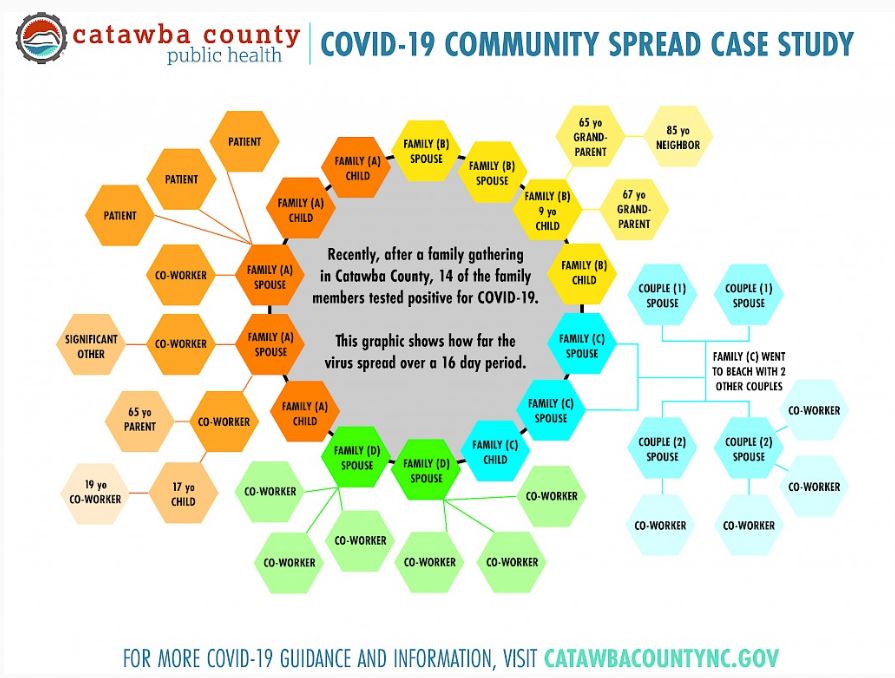
From the Catawba County posting about this:
Situations like this have become painfully common in Catawba County. I share this example because I hope it can help our community see how easily COVID-19 is actively spreading. More importantly, I hope it will convince us all to be even more willing to do the small things we’re being asked to do to protect ourselves and others: wear a mask in public, maintain physical distance, and wash hands frequently.
It’s not hard to prevent the spread COVID-19. What’s hard is having to call 20, 30, 40 people a day and tell them that not only are they sick with an untreatable illness, but they are also required to isolate themselves from others, including their loved ones, and stay home from work for two weeks or until they recover. This is especially difficult when they do not have the support systems that many of us take for granted, such as paid sick leave, the ability to isolate in their own home, or available caretakers for their children. It’s even harder when they are experiencing severe illness as a result of their exposure – exposure that could have been prevented.
Jobs Retained by PPP in the Triad’s 3 Big Cities
Digging a little more into the PPP numbers from the SBA (see yesterday’s post) it’s interesting to look at the number of small loans (under $150,000) versus the number of larger loans (over $150,000) and the number of jobs they have retained according to the report.
According to the data there were 9,670 loans combined in the three cities and of those 8,131, or 84% were under $150,000.

The data also shows that there were 115,448 jobs retained and of those 38,735, or 34% came from the small loans.

Spread
This New York Times interactive piece offers a chilling look into how COVID-19 spread in the US earlier this year. This part, in particular, caught my attention:
HOW THE FIRST OUTBREAKS SPREAD
Top federal health experts concluded by late February that the virus was likely to spread widely within the United States and that government officials would soon need to urge the public to embrace social distancing measures, such as avoiding crowds and staying home.
But Mr. Trump wanted to avoid disrupting the economy. So some of his health advisers, at Mr. Trump’s urging, told Americans at the end of February to continue to travel domestically and go on with their normal lives.
And they did. Millions moved across the country, cellphone data shows. Some unknowingly carried the virus with them.

Travel volume from March 1 to March 14, based on aggregated data from Cuebiq, a data intelligence firm. Minor routes not shown.
The reason this caught my attention is that in the March 1-14 window I traveled from my home in North Carolina to Washington, DC for a business trip that included a visit to the offices of several legislators on Capitol Hill on March 11. If that date looks familiar it’s because that’s the last day that Congress was open to visits from the public. Every office we visited had signs on the door stating that they were discouraging shaking hands, but that didn’t stop at least one Congressman from shaking my hand and one staff member from shaking everyone in my group’s hands – around 10 people.
In addition to visiting the Hill, I was attending a small national industry conference held at the Grand Hyatt. Several hundred people flew in from around the country for that meeting, and we spent hours together in meeting rooms of various sizes over several days. At the beginning of the conference, the only precaution we took was making sure everyone had hand sanitizer and we refrained from shaking hands. Three days later they had set up AV equipment in the meeting rooms so that people could remote in from their hotel rooms if they weren’t comfortable meeting in person.
After the conference, we were informed that if anyone was diagnosed with COVID-19 we would be informed and we never did get that notification. To be safe I decided to work from home for two weeks so I didn’t put my office mates at risk, and of course, by the time that was done, we’d shut down our office and moved everyone to work-from-home status.
In an interesting coincidence the League of Municipalities had a meeting in DC the same week we were there. Several members of Winston-Salem’s city council were there and visited Capitol Hill on the same day we did, March 11. Less than a week later they announced that they were self-isolating because attendees at their conference had tested positive for the virus. If I’d had any question about working from home before that then I’d have made the call to do so then because our paths crossed on the Hill.
So, how many meetings/conferences like ours were held somewhere in the country those first two weeks of March? How many people attending those meetings unwittingly carried the virus home with them? How many were like me: they didn’t really want to go to the meeting, but felt they had to? If the government had come out earlier then those meetings likely wouldn’t have happened and we wouldn’t have had to make that decision. It’s impossible to know how many additional infections/deaths this delay led to, but I suspect it was a substantial number.
This final bit of info from the Times piece:
More than 22,000 deaths in the New York City area could have been avoided if the country had started social distancing just one week earlier, Columbia University researchers estimate.
About 36,000 deaths nationwide could have been avoided by early May had social distancing begun earlier, the estimates say.
When Perception Matches Reality
Since the COVID-19 crisis began one of the local testing centers here in Winston-Salem, NC has been located on Hanes Mall Boulevard near my home, and I’ve driven past it at least a few times a week throughout the crisis. For much of the first six-ish weeks of the crisis, I would either see no one out there, or just the health workers hanging out waiting for potential cases to drive in. Then a few weeks ago I started noticing cars in line with people waiting to be tested, and then more recently I saw those lines getting significantly longer. It was noticeable enough that I mentioned to Celeste, my better 3/4, that I wouldn’t be surprised if we started to see on the news that there were more cases in Forsyth County. Sure enough, over the last two weeks, we’ve seen a heavy surge in cases and we’re not alone as the entire state of North Carolina has seen an uptick in positive test results and hospitalizations. The following is from the Winston-Salem Journal:
Forsyth County has experienced its largest one-day spike with 97 new cases reported Thursday by the county Health Department. The previous daily high was 61 on May 14. The number of COVID-19 related deaths remained unchanged at nine.
The overall total surged to 1,160, which may signal that Forsyth has surpassed Guilford for having the third-most cases by county. The latest N.C. Department of Health and Human Services update, released at 11 a.m. Thursday, had Guilford with 1,137 cases and 56 deaths.
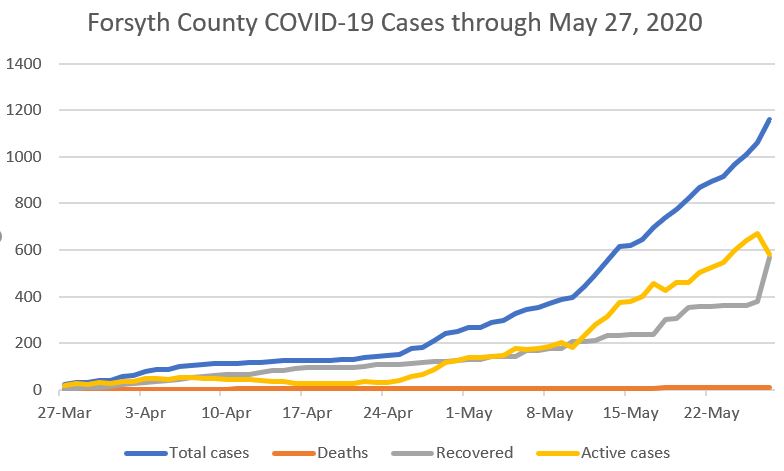
This is one of those times where I really wish the reality hadn’t matched my perception.
While we’re here I’ll also share that there’s an anomaly that I can’t wrap my head around: while Forsyth County’s case count has been skyrocketing the deaths have remained relatively low when compared to neighboring Guilford County. Forsyth has 1,160 total cases with 9 deaths, for a fatality rate of .775%. Guilford has 1,173 total cases with 56 deaths, for a fatality rate of 4.77%. Given that the two counties abut each other and are similar in so many ways I just don’t understand what can account for such a large discrepancy.
The numbers are tragic no matter how large or small, but it’s discrepancies like this that make me believe that we still don’t have an accurate picture of what this disease is doing to our community. Only time and good public health science will give us a true picture, and I fear that the worst of this picture is yet to be revealed.
Stories by the Numbers
Some interesting numbers. First, check out this graphic from today’s (May 8, 2020, 1:00 p.m.) Wall Street Journal website that highlights why the stock market is a pretty lousy proxy for the economy:

This next number caught my eye because it features a small Nebraska city, Grand Island, where Celeste and I spent one night last summer when we were driving home from Colorado. It’s from an article in the May 7, 2020 Wall Street Journal:
Local officials have now confirmed hundreds of coronavirus cases, with more than 200 linked to a local JBS USA beef plant and another 40 to area nursing homes. There were 1,228 Covid-19 cases as of Tuesday in a city of roughly 51,000, according to the regional health department. That puts its per capita rate of infection well above that of New York, the hardest-hit state in the nation by the coronavirus pandemic.
Compare those numbers to my hometown of Winston-Salem, NC, which has a population of 246,000, 347 confirmed COVID-19 cases and five deaths as of 5/8/2020. So despite have five times the population of Grand Island, Winston-Salem has had less than a third the number of confirmed cases. One interesting piece of info though: Winston-Salem has seen a recent spike in cases and a high percentage of those cases are tied to people who work in a Tysons Food poultry plant located in a county that’s an hour away.
Long story short: food processing plants are becoming a significant hotspot in the less urban parts of the country, and since those operations are all essential and can’t be done remotely, it wouldn’t be a stretch to think that small cities and towns across the country could see a significant per-capita impact for months into the future.